Jenna’s Blog – Revealing All About DIBH


Jenna Dean is a radiation therapist based at Port Macquarie on the NSW Mid-North Coast. She is a passionate advocate for rural patients receiving access to radiation therapy and a member of the Targeting Cancer Working and Advisory Group. She grew up in the NSW Hunter Valley and her interests include research, imaging, new technology, cross fit and photography.
In this blog she explains how breath hold techniques work for patients undergoing radiation therapy:
You may have very occasionally seen news headlines covering the latest developments in radiation therapy treatment and thought to yourself, ‘that’s great! better treatment for cancer patients’. BUT… what does that actually mean?
There is so much research and development going on in radiation therapy land. Innovative techniques are being developed, allowing us to provide more accurate, more effective treatment with less side effects. Winning!
After prostate, the next most common treatment site that benefits from radiation therapy is breast. Like prostate cancer, there are some important organs that don’t really like receiving too much radiation in that area such as the lungs and heart (more important on the left side). The way we traditionally treat this area already limits the dose to these important structures, but newer technologies now allow us to protect them even more. Introducing – Deep Inspiration Breath Hold (or DIBH as it is also known).
There are a few different ways to treat patients using breath hold techniques. Some of them involve placing a marker on the patient’s chest and when they have taken a breath and are holding in the right position, the machine will deliver their treatment. Other options involve the use of a ‘snorkel’ and nose peg with a machine that will help the patient to hold their breath with a certain amount of air in it. So once again, the patient will receive their treatment when this lines up perfectly.
The reason that this technique helps with treatment delivery is that it makes a mobile target a static one, so it removes the effect of motion (breathing is very important!), with the added benefit of making the breast or chest wall further away from the heart. This allows the radiation therapy team to ensure that the heart is receiving less dose while making sure we cover the breast tissue that we need to treat.
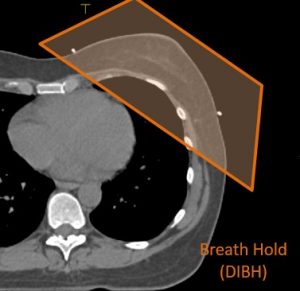
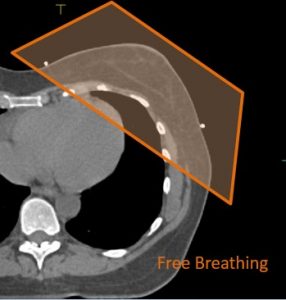
Check out these two pictures which may help explain it better:
The first picture shows the patient breathing normally, the second picture shows the patient taking a breath in and holding. This pushes the chest away from the heart so it gets less dose during treatment.
Make sure you check out the Targeting Cancer website for more information on radiation therapy.